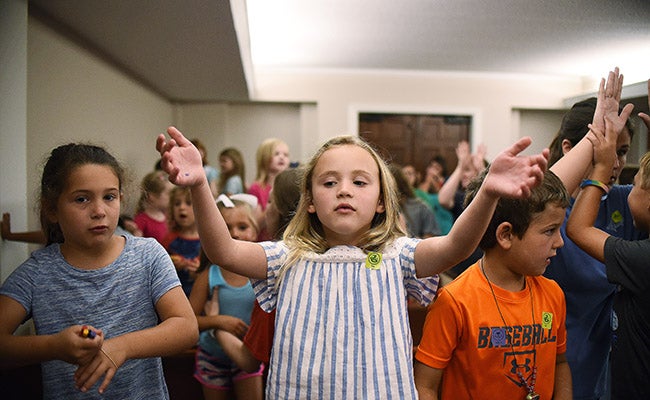Hospital CEO says county has two options: sell it or close it
Published 12:01 am Saturday, September 7, 2013

Ben Hillyer / The Natchez Democrat — Natchez Regional Medical Center CEO Bill Heburns addresses the crowd of supervisors, residents and hospital employees during the county’s public hearing on the possible sale of the hospital. During the meeting Heburn said he believes the hospital will either be sold or closed in two years.
NATCHEZ — Natchez RegionalMedical Center will close in two years if it isn’t sold, CEO Bill Heburn told residents Friday.
Heburn gave the ominous warning during the public hearing about the potential sale of the hospital.
Much of the discussion from hospital and county officials at the hearing was a retread of what has been said in recent weeks — small, independent rural hospitals can’t recruit the doctors they need and will have significant trouble bringing themselves in line with federal regulations coming down the pipeline.
- Ben Hillyer | The Natchez Democrat — Adams County resident Chuck Fields asks a question during Friday’s public hearing.
- Ben Hillyer | The Natchez Democrat — Susan Kings expresses her concerns about the effect the sale of the hospital will have on employee retirement.
- Ben Hillyer | The Natchez Democrat — Adams County Board Supervisor Mike Lazarus talks during the public hearing.
- Ben Hillyer | The Natchez Democrat — A video presentation led off Friday’s hearing at the Adams County Board of Supervisors board room.
- Ben Hillyer | The Natchez Democrat — Natchez Regional CEO Bill Heburn addresses the standing room only crowd at the public hearing Friday.
- Ben Hillyer | The Natchez Democrat
- Ben Hillyer | The Natchez Democrat — Susan King points to Natchez Regional lawyers and officials as she expresses her concerns Friday.
- Ben Hillyer | The Natchez Democrat — Natchez Regional board attorney Walter Brown speaks during the hearing.
- Ben Hillyer | The Natchez Democrat — Natchez Regional CEO Bill Heburn addresses the crowd.
Residents have also been leaving the area to find treatment elsewhere, they said, and doctors entering the health care field now want to work as part of a larger health care system.
But when area resident Felicia Hobbs said she was concerned that the hospital had been reported to be spending out of its recent settlement with Quorum Health Resources to make payroll, the hospital CEO was frank.
“I hear ‘Get out while you can,’ I hear ‘We can’t sustain (the Public Employees Retirement System),’” Hobbs said. “What is our timeframe for this and is there a possibility the hospital will close if we don’t sell?”
Heburn responded, “In my opinion, the hospital will close (in) less than two years.”
The Affordable Care Act is changing how hospital payments are structured, Heburn said, and is geared to fewer patients having to stay in the hospital. Under that model, NRMC can expect to see a 29-percent decrease in inpatient and a 17-percent decline in outpatient business, he said.
“You can’t sustain that,” Heburn said. “That is why you have to get a new group in here.”
“This year, we have almost a million dollars in unplanned plant problems in keeping the hospital running,” he said. “We spent $875,000 last year getting ourselves out of the 1980s and almost current with our computer systems.”
NRMC ultimately needs a new hospital building, Heburn said, but the hospital could operate for the next 30 years and never create enough equity to build that facility, which would cost approximately $150 million.
“This July and last July we have suffered another $300,000 reduction in our revenue,” Heburn said.
The current facility will likewise require a $5 million investment between now and 2017 to keep the wiring, plumbing and air conditioning working, he said.
When resident Kathy Traina asked what kind of guarantees the county will get that the ultimate buyer will build a new hospital facility, NRMC board of trustees attorney Water Brown said the bidding process will be structured in a way to encourage it.
“If nobody says they are going to build a new hospital, they are going to have to bid a lot higher,” he said.
Supervisor Mike Lazarus said bidders would have to file a security with the county that will likewise encourage the buyer to build.
“There will be a $10 or $15 million bond that they have to set aside, and if they fail to build a new hospital, that bond goes to the county,” he said.
When Traina asked about the possibility that the buyer could replace the hospital with a newer but much smaller facility of only 25 beds, NRMC’s Director of Physician Relations and Recruitment Sarah Smith said it wouldn’t make sense for a hospital system trying to capture the area’s health care outmigration to build such a small hospital.
Others at the hearing were concerned about the future for the hospital’s 400-plus employees. Resident Susan King said she was especially concerned about long-term employees in the PERS system.
“What about those who have only a couple of years left (before retirement)?” she said. “I don’t think y’all would like if your PERS system was yanked out from under you.”
Supervisors’ attorney Scott Slover said negotiations with potential bidders included the retention of employees and that those who were vested in PERS would have some options.
But Supervisors’ President Darryl Grennell expressed sympathy for those who were late in their careers.
“I am a professor at Alcorn (State University), and if the state decided it no longer wanted Alcorn and sold it to a private institution, personally I would go to Franklin County or some place with PERS and beg them for two years sweeping the floors or whatever,” he said.
But while NRMC Director of Communication Kay Ketchings said she was concerned about the future, she thought the players should take a look at the bigger picture of what the hospital sale could mean for the area as a whole.
“We are concerned so much so for the process and what is for the betterment of Natchez and health care that you (choose to) put aside your personal investment in it such as PERS,” Ketchings said. “Sure you would all stay in PERS if you could, but we don’t expect the hospital to limp along until we get two more years. I may not even have a job when this happens, but I hope Natchez gets what it deserves to get.”
King likewise expressed discomfort that the county would move forward with the sale without the supervisors knowing the amount of the hospital’s settlement with QHR. The settlement was reached on November 2012 and was sealed in court.
NRMC had sued QHR — its former management company — alleging mismanagement by QHR had ultimately forced it into bankruptcy in 2008. The original lawsuit was for $44 million.
Lazarus said the supervisors had consulted with the state ethics commission and found out that if they were told the details of the settlement, they would be obligated to tell the public.
“The law says that if I know a secret, you know it,” Lazarus said. “The ethics commission said that I cannot keep that secret.”
The president of the hospital trustees, the Rev. Leroy White, said the punishment for divulging the amount of the settlement to someone who could not sign a confidentiality agreement was jail.
Brown said that QHR had been willing to double the settlement if NRMC would seal it.
Slover said that no matter what the amount of the settlement was, it wasn’t enough to address the hospital’s ultimate needs.
“To build a new hospital you need a cashflow of $140 million, and the original lawsuit was for $44 million,” he said. “You are still $100 million shy even if they settled for everything, which is unlikely.”
Resident Chuck Fields said he was concerned that Heathcare Management Partners had been contracted to help sell the hospital. HMP was hired in 2008 to sell NRMC but was not successful at the time.
Fields said he did not believe the 2008 process was open enough to public scrutiny.
“If you don’t look back and learn from your mistakes, you are prone to make the same mistake again,” Fields said. “I think this warrants a little looking back at who is involved in this — I don’t think anybody in here is rushing into decisions without thinking they are doing the best thing for the community and health care in the community, but my fear is we will have another process cloaked in secrecy.”
“The sale of a hospital has got to be a transparent process.”
Fields also asked if anyone present at the hearing was involved in what is to be the opening salvo of bidding, the negotiation of a stalking horse bidder.
In a stalking horse bid process, a bidder negotiates with the county a minimum bid to purchase the hospital. If no higher bid is made when the hospital goes to auction, the stalking horse is automatically the buyer.
Brown stated that he and Slover were involved in reviewing legal documents prepared in the negotiations, but that they were not involved in the actual negotiations. Heburn likewise said he was not involved in the negotiations but had previously met with some of the parties the hospital approached about being stalking horse bidders.
Brown said instead that HMP was leading the negotiations, and that HMP Chief Executive Officer Scott Phillips was not able to be in Natchez Friday because he was testifying as a witness in a trial in South Carolina.
Phillips was scheduled to be in Natchez for the original date set for the public hearing, Brown said.
The first date for the public hearing was set for mid-August, but had to be rescheduled because the legal advertisement announcing the meeting did not run enough times prior to the hearing.
Brown said that of the six health care systems the hospital has approached about being a stalking horse, two have not shown much interest and two have shown active interest.
In an open letter from the Homochitto Valley Medical Society, Dr. Roderick Givens said the HVMS would prefer to see Natchez become a single-hospital town because having two acute care hospitals in the area divides resources.
The HVMS supports a new hospital structure in the area, Givens wrote, because both existing hospitals have serious limitations in their physical plants and campus sizes.
The HVMS opposes, however, the idea of NRMC being taken over by an outside health care system and being used only to feed patients who could be treated locally into out-of-town systems.
“We as physicians are not concerned with who owns or operates a single hospital facility here, only that there is a single hospital here and preferably a new one,” Givens said. “Further, we hold that we as practicing physicians in Natchez, dutifully serving this region, are able with the right circumstance to bring in more specialists who will work and live right here as members of this wonderful community.”